MakeBirthEasier
Make Birth Easier Campaign for mums, for babies and for midwives
Make Birth Easier Supports Optimal Cord Clamping
An excerpt of this article was published in
The National Childbirth Trust (NCT) magazine in December 2015.
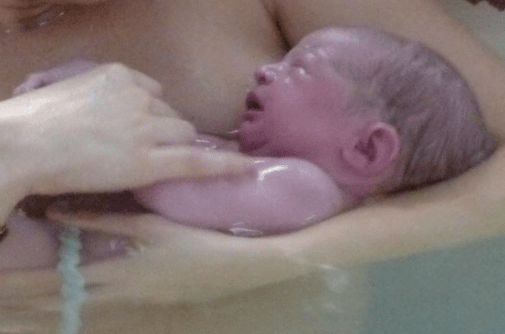
‘Delayed Cord Clamping – The single most important gift you can give to your baby.’ Hannah Tizard #BloodtoBaby
Make Birth Easier
Blogging has been quiet for a few months since the launch of Make Birth Easier Campaign UK earlier this year, however, progress has not halted and with continuing support, the Campaign message – Fetal Navigation Techniques for easier birth, to be included in the standard training curriculum for all midwives – is reaching further and further around the world.
See below for links to previous Make Birth Easier posts including The Actually Useful, Very Sensible and Practical Guide to Make Birth Easier.
In this post, I focus on one of the greatest gifts you can give to your baby…
Optimal Cord Clamping – One of the Greatest Gifts to Your Baby
Pregnant for the first time and like many new mums, I had concerns about the health of my baby. Will she be born healthy? What can I do to give her the best chance of a healthy body and mind? Many mums find themselves dwelling on these and many other questions. Advice is plentiful and it can feel as if there are so many choices and considerations.
My Hypnobirthing teacher discussed several health topics with me including healthy eating, drinking plenty of water, appropriate exercise, and avoiding alcohol and caffeine. These are the basics of a healthy lifestyle of course and always advised during pregnancy. She also went through more specific options for our birth preferences including fetal positioning techniques to help labour progress more easily, different levels of monitoring available for baby during labour, limiting the number of vaginal examinations, and whether we would choose vitamin K by mouth or injection. I was very interested learning about these things and what they meant for me and my baby.
One particular thing she brought up which really caught my attention was Optimal Cord Clamping (OCC), also referred to as Delayed Cord Clamping (DCC). I had never heard of this before. I suppose it had never really occurred to me that anything different would or could be done with the umbilical cord other than the classic image I’d seen in movies and on TV. You will probably recognise the scene – where the cord has to be cut immediately as if it’s some kind of an emergency situation in itself.
So, doesn’t the cord have to be cut immediately after birth? Actually, in most cases, no it doesn’t.
Really?
This notion seemed very strange to me. If it’s not a necessity, then why on earth would it be done routinely for as long as many people can remember?
The procedure of cutting the cord immediately started in the 1960-70s with the introduction of drugs which reduce the incidence of post partum haemorrhage i.e. preventing the mum from bleeding significantly after birth. Great for mum – yes absolutely! Still, clamping and cutting the cord immediately was done with no consideration for the effect this would have on the baby and there is actually no evidence at all to support this practice today. It has become so normal that many presume it has to be done that way.
When I started asking questions, I realised that of course for the duration of its life inside mum, baby’s blood has been distributed between its body and the placenta. Research has shown that clamping and cutting the cord immediately means that one quarter to one third of the baby’s blood is left in the placenta and cord. WOW. That means that baby is missing up to 30% of its own blood and all the oxygen that goes with it. I was shocked!
I remembered donating a pint of blood and being told to rest for 15 minutes (or as long as I needed) with a drink and a snack before being allowed to get up and leave. That is just one pint of my blood. As a grown woman I usually have around 8-10 pints of blood inside me. I’m fairly tall so let’s say 10 pints. So I donated about 10% of my blood and looked rather grey and felt pretty wobbly. Imagine being born, at your most vulnerable moment in life, deprived of 30% of your intended blood volume… No wonder babies are often born in a weakened state!
My initial reaction was “I want my baby to be born with all its blood please!”
Then doubts came back to me…What if the cord is around the neck? Baby won’t be able to breathe! Then the realisation dawned on me during further discussion that baby doesn’t need to use its neck to breathe oxygen until the umbilical cord has been clamped. If the cord is pulsating, then the placenta is still attached and both the cord and placenta are still functioning; oxygenated blood is still being pumped around baby’s body.
The cord being around the neck once or even twice, it seems, is a fairly common occurrence, and while the cord is still functioning, this usually causes no problems. The message here is, if the cord is still pulsating, delay clamping and cutting while the cord is unwrapped from around the neck! Thankfully this is now taught in midwifery training, in some areas of the UK at least.
Of course there are cases where it might not be appropriate to delay clamping of the cord. These include; if the umbilical cord is compromised somehow, i.e. damaged or compressed, if the cord or the baby has a heartbeat below 60 beats/minute that is not getting faster, and also if mum is bleeding significantly (postpartum haemorrhage). These would be reasons to clamp and cut the cord early. In many other cases, if baby is struggling, it will benefit most from receiving more of its full intended blood volume.
If cord blood gases need to be taken, they can still be taken from a pulsating cord with a small needle. Levels of specific gases in cord blood can give an indication of the health of the baby and taking a sample from a clamped and cut cord is often standard procedure for high risk births. Doctors requiring a sample of blood gases is frequently stated as a reason for immediate cord clamping but gases can be taken from an unclamped cord. By using a small needle to take the sample (similar to when you have a blood sample taken from your arm), there is no need to clamp and cut.
A resuscitaire trolley called the ‘Bedside Assessment, Stabilisation & Initial Cardiorespiratory Support’ (BASICS) trolley was redesigned several years ago which now makes it possible not to have to choose between resuscitating a baby and delaying cord clamping. Resuscitation can be immediate and at mother’s side while the cord is intact which gives the baby potential for the greatest benefit. The team who redesigned the BASICS trolley received the Medical Futures Innovations Award in 2011 (Best Service Redesign in Cardiovascular Innovations) for their work on it. The BASICS trolley is called the Lifestart and has been produced by Inspiration. As more and more hospitals start to use the Lifestart trolley, many, many more babies will benefit.
The benefits of Optimal Cord Clamping are many and include; improving the adjustment the baby’s heart and lungs make from being a fetus to being a breathing baby (because of the increased blood flow to baby’s vital organs in those first moments), improving iron stores up to 6 months, reduced instance of iron deficiency anaemia, higher red blood cell flow to vital organs, increased duration of early breastfeeding (I can only imagine this is due to baby being generally stronger from birth), increased white blood cells (leading to better infection prevention, including umbilical infections), less blood spatter (which in countries with high instance of blood borne disease such as HIV and malaria equates to prevention of disease transfer) .
 Research shows that babies can gain up to 214g in the first five minutes following birth if the cord is left unclamped. Cord blood has also been shown to contain a very high concentration of stem cells, important in development throughout the baby’s entire lifetime. There is a possible risk of jaundice which requires treatment by phototherapy and this must be weighed against the benefits of optimal clamping. Benefits for preterm and very preterm (premature) babies are huge. OCC leads to substantially lower rates of some life threatening issues.
Research shows that babies can gain up to 214g in the first five minutes following birth if the cord is left unclamped. Cord blood has also been shown to contain a very high concentration of stem cells, important in development throughout the baby’s entire lifetime. There is a possible risk of jaundice which requires treatment by phototherapy and this must be weighed against the benefits of optimal clamping. Benefits for preterm and very preterm (premature) babies are huge. OCC leads to substantially lower rates of some life threatening issues.
For the mother, optimal clamping does not increase the risk of postpartum haemorrhage. Allowing the umbilical cord to stop pulsating also contributes to the placenta being able to detach from the uterus more safely and efficiently, so this in itself reduces the chance of significant maternal bleeding. Interestingly, early breastfeeding is also known to help the placenta to detach properly and to reduce the occurrence of bleeding from mum. Many midwives are waiting until after the cord has stopped pulsating to administer the hormonal injection (usually syntocinon these days) which helps the placenta be born more quickly as part of an actively managed third stage of labour.
There is no reason why, in most cases, OCC cannot occur also as part of a caesarean section too. Baby can be placed between mums legs for vital skin to skin while the umbilical cord is allowed to complete its job. This also helps baby be exposed immediately to mums good bacteria, so important to help baby build a strong immune system (‘Seeding the Microbiome’, which uses mother’s natural healthy bacteria -from vagina, skin to skin and breastmilk – to colonise the baby’s gut, as would be the case for a vaginal birth, is a subject worthy of a whole article all of its own so watch this space!).
So why in many hospitals is the umbilical cord still being cut immediately as a matter of routine? The truth is, it has been a very long battle to gain recognition of the benefits of delaying clamping of the cord to allow placental transfusion. Due to much campaigning by some amazing midwives and doctors from the UK and around the world, thankfully there is now extensive evidence available for both term and preterm babies, and recognised international and British bodies such as the World Health Organisation (WHO), the International Liaison Committee on Resuscitation (ILCOR), the Royal College of Midwives (RCM), and the Royal College of Obstetrics and Gynaecologists (RCOG), in addition to the National Institute for Health and Care Excellence (NICE) Guidelines now include for Optimal Cord Clamping.
British and international guidance now recommends that the umbilical cord should be left intact for at least a minute based on a clinical assessment of the situation. Since 2014 the NICE Guidelines make this recommendation unless there is a concern about the integrity of the cord or the baby has a heartbeat below 60 beats/minute that is not getting faster, which is very rare.
Many hospitals are changing their procedures to include at least some delay in clamping the umbilical cord, although it is still taking time to filter through. There are not yet that many hospitals with specific OCC guidelines in place and there is still a lack of evidence based recommendations for the timing of umbilical cord clamping. Hospital guidelines range from 1, 2, or 3 minutes and some allow the cord to stop pulsating. In other hospitals OCC is something you, as mother, need to state as part of your birth preferences.
As an example, my own birth preferences (otherwise known as a birth plan) stated the following: ‘DELAY CORD CLAMPING and cutting for minimum 3 minutes or UNTIL AFTER PULSATION HAS CEASED (unless baby’s heartbeat <60bpm without increasing, or, there is significant maternal haemorrhage). If cord gases need to be taken, please do so with a small needle so delay in clamping can occur. In event baby is compromised she will benefit most from receiving placental blood transfusion. If the cord is pulsating, the placenta is still attached and both are still functioning’.
One of the barriers to Optimal Cord Clamping not yet being routine in hospitals is that some hospitals have interpreted that OCC is only suitable for healthy women and not suitable for any women categorised as ‘high risk’. This is due to the NICE guideline on OCC being included in the section for healthy women and babies. Hospitals can have rigid policies for categorising women and consequently may practice Immediate Cord Clamping (ICC) on healthy women and babies who have been given a ‘high risk’ label (induction, Vaginal Birth After Caesarean, continuous monitoring…). Research shows OCC presents no risks to women, whether high risk or low risk, and it actually benefits compromised babies. It is precisely these babies who are struggling that frequently need Optimal Cord Clamping even more in order to give them the strength to recover or even survive. Immediate Cord Clamping is not evidence based. Whatever category women fall under it is important for women to tell their birth attendants that they want their baby to have Optimal Cord Clamping.
One British Consultant-led Midwife Unit introduced Optimal Cord Clamping guidelines for ALL babies, regardless of delivery and included for a team of Advanced Neonatal Nurse Practitioners (ANNP) to work with the midwifery/obstetric teams to ensure benefits from OCC. The Unit conducted a review to see if these guidelines were being put into practice. The findings were startling. The introduction of OCC resulted in a significant reduction in the number of babies born there receiving resuscitative measures at birth. The Unit very much supports the practice of ‘assisted transition’ from placental to pulmonary respiration (transition from oxygen via the umbilical cord to breathing with the lungs). In short – delaying the clamping and cutting of the cord means that fewer babies need help to breathe.
The miracle moments of birthing my daughter, and then my son, into water, brought home to me the still ingrained fear I had of the baby needing to breathe immediately. Both were under water for what seemed like an eternity. First the head was born, then each baby took a minute or so to turn to allow the body to be born. During these few minutes under water the previously held anxiety in me reared its head for a moment that baby needed to breathe, but of course, in reality the baby is absolutely fine underwater (as I was reassured by my lovely midwife). It has spent the whole of its life inside mummy in fluid and never yet used its lungs. For both my children I chose to delay cord clamping until the umbilical cord had stopped pulsating and was empty and white #Wait4White.
It is now recognised that best for baby is to give it time to start using its lungs properly before the cord is clamped (assisted transition). Give it time to receive its full quota of oxygenated blood. Baby will be much stronger for it in those first few vulnerable moments of life after birth. Incredibly, this fact has been written about by scholars for thousands of years. Aristotle 300BC “Frequently the child appears to be born dead or it is feeble but before the tying of the cord, a flux of blood occurs into the cord and adjacent parts…and at once the baby, who had previously been as if drained of blood, comes to life again.
Optimal Cord Clamping saves lives. Share this message.

Blog written by Alix Fernando – founder of Make Birth Easier Campaign UK. https://makebirtheasier.wordpress.com/ https://www.facebook.com/makebirtheasier/
#MakeBirthEasierCampaignUK #SpinningBabies
With very special thanks for the assistance of Amanda Burleigh – Optimal Cord Clamping campaigner, SHCR Change Agent, OCC/Full Blood Benefit Facebook page founder and Midwife of the Year for several years running with various bodies including the British Journal of Midwifery. Medical Futures Innovations Award in 2011 for BASICS trolley with the basics team. See also #Wait4White.
For further information please see Optimal Cord Clamping campaign #BloodtoBaby by Hannah Tizard, RCM shortlisted Evidence into Practice Award 2016, UCLan student midwife, National OCC Working Group member. Order free educational resources for midwives, childbirth practitioners, women and families from www.bloodtobaby.com
Make Birth Easier Blogs
1. Click here for the story behind the Make Birth Easier Campaign and find out about how I used fetal navigation techniques to have two straightforward, intervention-free labours against the odds.
2. Click here to learn more about the research we so need into fetal navigation techniques to prove they are safe and effective.
3. Click here to learn about how moving mummy helps baby to move into a better position for easier birth and how the medicalisation of birthing over the years has ignored gravity and movement.
4. Click here to read about the dramatic difference that using fetal navigation techniques for easier birth can make to thousands of women by reducing the need for aftercare, both in terms of post operative care, and also mental health issues such as Post Natal Depression (PND) and Post Traumatic Stress Disorder (PTSD).
Make Birth Easier blog written by Alix Fernando – founder of Make Birth Easier Campaign UK.
https://makebirtheasier.com/ https://www.facebook.com/makebirtheasier/ @MakeBirthEasier #MakeBirthEasierCampaignUK #SpinningBabies
The contents of this blog are not intended, and should not be read as constituting medical advice, diagnosis or treatment. Always consult your doctor, midwife or other qualified healthcare provider before making any changes to your birth plan or your recommended routine.